S Jay Mathews
The TASTE and TOTAL studies suggested that routine thombus aspiration in patients undergoing percutaneous coronary intervention (PCI) did not provide mortality benefit and may increase the risk of stroke. However, a new study (CHEETAH) is evaluating whether a next-generation aspiration catheter could lead to improved outcomes. S Jay Mathews (Manatee Memorial Hospital, Bradenton, USA), principal investigator of the study, talks to BIBA Briefings about why thrombus aspiration still has potential as an effective tool in PCI.
What did the TOTAL/TASTE studies indicate about the use of aspiration thrombectomy for removing thrombus in coronary vessels?
Published in 2013, TASTE randomised patients with ST-segment elevation myocardial infarction (STEMI)—with or without thrombus—to percutaneous coronary intervention (PCI) alone or manual aspiration followed by PCI. The outcome was that aspiration showed no benefit when compared to the PCI alone group and no difference in all-cause mortality.
TOTAL, published in 2015, also studied patients with STEMI, with or without thrombus, randomised to PCI alone vs. manual aspiration followed by PCI. The outcome of TOTAL was that routine aspiration showed no benefit and there was an increased rate of stroke in the manual aspiration group within 30 days.
How have these trials influenced current guidelines on thrombectomy?
They led to changes in the guidelines. In 2011, the American College of Cardiology/American Heart Association (ACC/AHA) guidelines stated “manual aspiration thrombectomy is reasonable for patients undergoing primary PCI” (Class IIa). However, after the TOTAL trial, the guidelines were changed (in 2015) to: “the usefulness of selective and bailout aspiration thrombectomy in patients undergoing primary PCI is not well established” (Class IIb). They also state that “routine aspiration thrombectomy before primary PCI is not useful” (Class III). Therefore, as per the guidelines, the selective use of aspiration thrombectomy may be worthwhile in patients with high thrombus burden. That is what we are currently seeing in clinical practice.
Why, despite the findings of TOTAL, is there still interest in thrombus aspiration?
One major limitation of PCI without aspiration for acute coronary syndromes is microvascular obstruction of the infarct related artery because of downstream embolisation of thrombotic material. This can result in no-reflow phenomena and continued myocardial infarction. Moreover, in high thrombus burden, the true severity of the lesion may be obscured. There often may be a column of thrombus or stasis of blood prior to the culprit lesion. The strategy of upfront ballooning to restore flow may result in injury to healthy vessel and require longer stent lengths during PCI. High thrombus burden patients often require more expensive pharmacologic agents such as glycoprotein IIb/IIIa inhibitors just to help reduce clot. These patients also tend to be sicker, requiring monitoring in intensive care post-procedurally.
In 2018, the TOTAL authors studied a subset of patients with high thrombus burden from the trial. They found an increased rate of stroke in the high thrombus burden patient subset, but with a reduction of distal embolisation. They concluded: “There may be a potential for future thrombus removal devices to reduce mortality if they are able to avoid an increased stroke risk. Further innovation and research are needed in this high-risk population.”
Therefore, PCI with thrombectomy has been regaining increased attention as a way to mitigate high thrombus burden. Adjunctive therapies such as CAT RX (Penumbra) can help address the thrombus in coronary vessels during PCI as is being studied in CHEETAH.
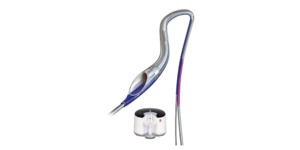
CAT RX
What are the aims of the new CHEETAH study?
The CHEETAH study aims to evaluate initial safety and collect performance data for Penumbra’s Indigo aspiration system with the CAT RX aspiration catheter, when used as an adjunctive device prior to standard of care PCI in patients with high thrombus burden in coronary vessels.
How is this technology different from the technology assessed in the TOTAL trial?
Clinical evidence has shown that aspiration thrombectomy is capable of removing thrombotic material from occluded coronary arteries. This may improve thrombolysis in myocardial infarction (TIMI) flow and possibly prevent no-reflow phenomenon. Early evidence suggested a reduction in major adverse cardiovascular events, although larger randomised clinical trials using routine aspiration for all myocardial infarction patients were unable to confirm those results. All prior thrombectomy trials used small volume (e.g. 30 cc) syringes using catheters with smaller lumens. Manual aspiration also suffers from decreased aspiration force as the syringe fills with fluid. With inconsistent vacuum, there is decreased efficacy and a potential for systemic embolisation during catheter removal. This phenomenon was reported in the TOTAL trial in 2015 and led to the decline in the use of aspiration thrombectomy in acute coronary syndromes. Subgroup analysis exploring the high thrombus burden subset of patients highlighted the potential for improved outcomes with better technology. This has motivated further innovation in the field of coronary aspiration.
The aim of mechanical power thrombus aspiration is to deliver consistent suction throughout the aspiration cycle in order to maximise efficiency of thrombus removal. Removing thrombus from hard-to-reach vessels requires a highly deliverable, atraumatic catheter. With CAT Rx, Penumbra has adapted their neuro-tracking technology used in stroke intervention combined with their mechanical power aspiration system to address the limitations of traditional manual aspiration thrombectomy in coronaries.
Why might these differences lead to different outcomes than those seen in the TOTAL trial?
Just like the IMS-III trial for ischaemic stroke, the TOTAL trial highlighted that new therapies are needed to improve the outcomes of these patients with high thrombus burden. Early experience with CAT RX data was presented at American College of Cardiology (ACC) Scientific Sessions. These data showed both initial safety and efficacy for the CAT RX mechanical power aspiration catheter for thrombus removal in acute myocardial infarction patients. These results are very encouraging and to date, CAT RX has now been used in more than 5,000 patients with acute coronary syndromes. The CHEETAH study is the first step toward making coronary mechanical thrombectomy standard of care for high thrombus burden patients. We expect this study to refine our technique of thrombus aspiration and fine tune the use of the CAT RX for patients with high thrombus burden.
Which patients do you think could benefit the most from mechanical thrombectomy for thrombus removal in the coronary vessels?
Mechanical thrombectomy could potentially benefit patients with high thrombus burden in the coronaries. For the purposes of the CHEETAH study, we have selected to enroll patients with TIMI grade 4 and 5 thrombus.
What lesson can be learnt from the use of mechanical thrombectomy to treat acute ischaemic stroke?
The early experience with stroke intervention was disappointing. After the failure of IMS III, it took a group of dedicated neurointerventionalists, proper patient selection and advances in technology to pursue the MR CLEAN trial—which unequivocally established the benefit of mechanical thrombectomy for acute ischaemic stroke. We are currently in an era not dissimilar to this time period in the coronary space. For acute coronary syndrome patients with high thrombus burden, further innovation and research is needed for the benefit of this high-risk patient population.